By Dr Sumit Toor
Introduction
In the realm of facial cosmetic and reconstructive surgery, the primary goal is to enhance harmony and restore function while leaving as little evidence of the intervention as possible. For patients, especially those from Indian and international backgrounds with diverse skin tones, the quality of the resulting scar is often the most significant concern. While modern surgical techniques have advanced tremendously, the way a body heals is a complex biological process. While no surgeon can predict scar outcomes with 100% certainty, we use risk stratification to estimate the likelihood of adverse scarring and implement preventative measures accordingly.
Understanding the Difference Between Keloids and Hypertrophic Scars
It is common for patients to label any thick scar as a “keloid,” but in clinical practice, we distinguish between two primary types of abnormal scarring:
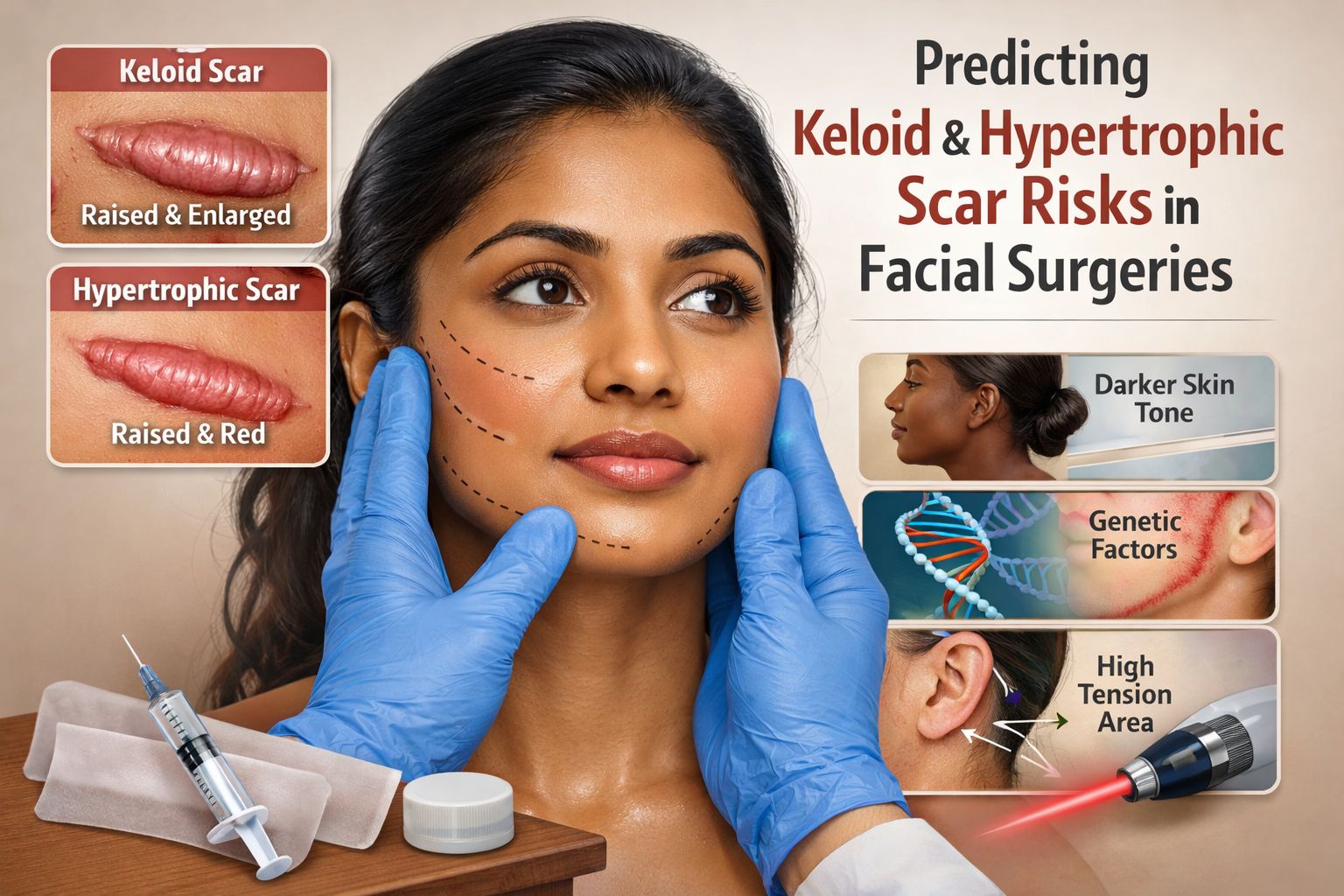
- Hypertrophic Scars: These are raised, red, and firm scars that remain within the boundaries of the original incision. They often develop within weeks of surgery and may partially regress or soften over several months to years.
- Keloids: These are more aggressive. A keloid grows beyond the original borders of the wound, invading surrounding healthy skin. They do not regress spontaneously and can be accompanied by itching, pain, or a persistent burning sensation.
Can We Predict Who Will Scar Badly?
Predicting scar formation is probabilistic rather than absolute. As a board-certified plastic surgeon, I evaluate a patient’s risk by looking at their biological blueprint and surgical history. While we cannot change your genetics, a thorough clinical examination allows us to identify “high-risk” individuals and tailor the surgical approach to minimize tension and inflammation.
Major Predictors of Keloid and Hypertrophic Scar Formation
Several factors influence how your skin will respond to an incision. Understanding these helps us set realistic expectations and plan postoperative care.
- Personal and Family History: The strongest predictor is how you have healed in the past. If you have existing keloids on your body, your risk for future ones is significantly higher.
- Skin Phototype: Patients with more pigmented skin (Fitzpatrick types IV, V, and VI), common in Indian and African populations, have a higher biological predisposition to keloids.
- Age: Younger patients (under 30) tend to have more active collagen production and higher skin tension, which can lead to more robust—and sometimes overactive—scarring.
- Anatomical Site: The face has varying risk zones. The mandible (jawline), preauricular area (front of the ear), and alar base (nostrils) are higher-risk zones due to movement and tension. Conversely, the eyelids and columella (base of the nose) generally heal exceptionally well.
- Wound Tension: Scars that are pulled tight are more likely to widen or become hypertrophic.
- Skin Quality: Thick, sebaceous (oily) skin is often more prone to visible scarring compared to thin, dry skin.
Preoperative Assessment by Plastic Surgeons
Before any facial procedure, a surgeon must perform a “scar audit.” This involves examining existing scars on the patient’s chest, shoulders, or back—areas where keloids are most common. We also discuss the patient’s ethnic background and family history. This assessment is vital for informed consent, ensuring the patient understands their specific risk profile before proceeding with elective surgery.
Surgical Strategies to Reduce Risk
The surgeon’s technique is the first line of defense against bad scarring. We employ several strategies:
- Relaxed Skin Tension Lines (RSTL): Placing incisions within natural wrinkles or skin folds to hide the scar and reduce tension.
- Layered Closure: Using deep sutures to take the tension off the skin surface, allowing the top layer to heal without being pulled apart.
- Atraumatic Handling: Using delicate instruments to avoid crushing the skin edges.
- Hemostasis: Ensuring there is no blood trapped under the skin (hematoma), which can cause inflammation and scarring.
Postoperative Scar Prevention Protocols
Healing doesn’t end when the sutures come out. For high-risk patients, we initiate a proactive protocol:
- Silicone Therapy: Silicone gels or sheets are the gold standard for flattening and softening scars.
- Sun Protection: UV exposure can permanently darken a healing scar (hyperpigmentation).
- Scar Massage: Once the wound is closed, gentle massage helps break up collagen bundles.
- Early Intervention: If a scar shows signs of thickening, we may use steroid injections or laser therapy to settle the inflammation early.
Facial Procedures With Relatively Higher vs. Lower Scar Risk
Not all facial surgeries carry the same risk. Blepharoplasty (eyelid surgery) is known for having some of the best-healing scars on the body because the skin is very thin and under low tension. Rhinoplasty scars (if external) are usually very well-hidden and heal well. However, Otoplasty (ear pinning) and Facelifts involve incisions in areas (like the back of the ear or the jawline) that are more prone to hypertrophic changes if not managed meticulously.
When Should Patients Avoid Elective Facial Surgery?
In some cases, the risk outweighs the benefit. Patients with a history of severe, multi-site keloids should approach elective facial surgery with extreme caution. Additionally, surgery should be delayed if there is uncontrolled acne or active skin infections in the surgical field, as inflammation is the enemy of a good scar. Finally, patients must have realistic expectations; surgery creates scars, and while we aim for them to be invisible, they are never truly non-existent.
Frequently Asked Questions
“If I had a keloid on my chest, will I get one on my face?”
Not necessarily, but you are at a higher risk. The chest is a high-tension area and much more prone to keloids than the face, but your biological tendency remains a factor we must respect.
“Can scar creams prevent keloids?”
Over-the-counter creams have limited efficacy against true keloids. Medical-grade silicone and professional intervention (like steroid shots) are far more effective for high-risk individuals.
“Should I avoid cosmetic surgery if I am keloid-prone?”
It is not an absolute contraindication, but it requires a specialized approach, meticulous technique, and a commitment to a strict postoperative scar management plan.
Conclusion
Predicting the perfect scar is impossible, but managing the risk is well within our reach. By combining a patient’s biological history with advanced surgical techniques and diligent postoperative care, we can achieve beautiful, natural results even in patients with higher risk profiles. Your biology provides the canvas, but the surgeon’s technique and your aftercare determine the final picture.
Anant Aesthetic Clinic, Adampur